S**t We Deal With Shorts: Time Burden with Dr. Jill Tirabassi
Live from Stage 4 | Episode # 022| 3/31/2026 | S**t We Deal With
Listen to full episode :
Host
Dr. Jill N. Tirabassi, MD, MPH
A sports and family medicine specialist, researcher, and educator based in Buffalo, NY. She is a Clinical Assistant Professor at the Jacobs School of Medicine and Biomedical Sciences and serves as the Health and Wellness Thread Leader at the University at Buffalo.
Professional Background
Specialties: Dr. Tirabassi focuses on Sports Medicine, Family Medicine, and Preventive Medicine.
Education:
MD: SUNY Upstate Medical University (2012).
MPH: University of Massachusetts (2019).
Research & Advocacy
Dr. Tirabassi is a researcher with a strong emphasis on Lifestyle Medicine and nutrition.
Key Projects: She has led initiatives such as "Developing School-based Food Literacy Initiatives for Buffalo Teens" and research into Food Prescription Programs for older adults.
Awards: She recently received the Food as Medicine Clinical Leadership Award(November 2025) for her work in primary care and implementation science.
Community Work: She is an advocate for those with Metastatic Breast Cancer (MBC), having served as a mentor with Project Life and an alumna of the Hear My Voice MBC Leadership program. She also co-hosts podcasts/discussions focused on breast cancer support.
Summary
How much time does living with metastatic breast cancer actually take? In this episode, Dr. Jill Tirabassi dives into recent research that puts real numbers to what many in the MBC community instinctively know: managing advanced cancer is incredibly time-consuming.
Jill examines a December 2025 JAMA Network Open Prospective Study which used a validated smartphone app (Daynamica) to track every cancer-related episode of care, travel, waiting, and at-home tasks for 78 adults with metastatic breast or advanced ovarian cancer over 28 consecutive days.
The research used mobile technology to document:
Out-of-home care: Patients averaged 4 cancer-related trips over 28 days (roughly once weekly), primarily for clinic visits and lab work
Wait times: While half experienced waits under 15 minutes, 14% waited over an hour—with some extreme cases reaching 2.5 hours
Travel burden: Average travel time was 35 minutes per appointment, often exceeding actual care time
Home tasks: Patients spent a median of 209 minutes weekly on cancer-related activities—medications, scheduling, billing, symptom monitoring
Daily disruption: Over one-third of participants reported cancer tasks disrupted their daily activities more than half the time
The Reality Check
Most participants spent 5-15 hours per week managing their cancer care—not quite the "full-time job" metaphor often used, but a substantial commitment nonetheless. Only two patients exceeded 25 hours weekly, though the burden varied significantly depending on treatment line and side effects.
Why This Matters
This study validates the invisible labor of living with metastatic cancer. Beyond scans and treatments, patients navigate complex logistics, financial administration, and constant health monitoring. Jill reflects on her own experience across multiple treatment lines—from easier oral medication periods to more demanding IV infusion schedules.
By documenting these realities, researchers help healthcare systems and policymakers understand what patients truly face—and hopefully identify ways to reduce these burdens.
Study Citation: "Time Burden in Patients with Metastatic Breast and Ovarian Cancer From Clinic and Home Demands," JAMA Network Open, December 2025
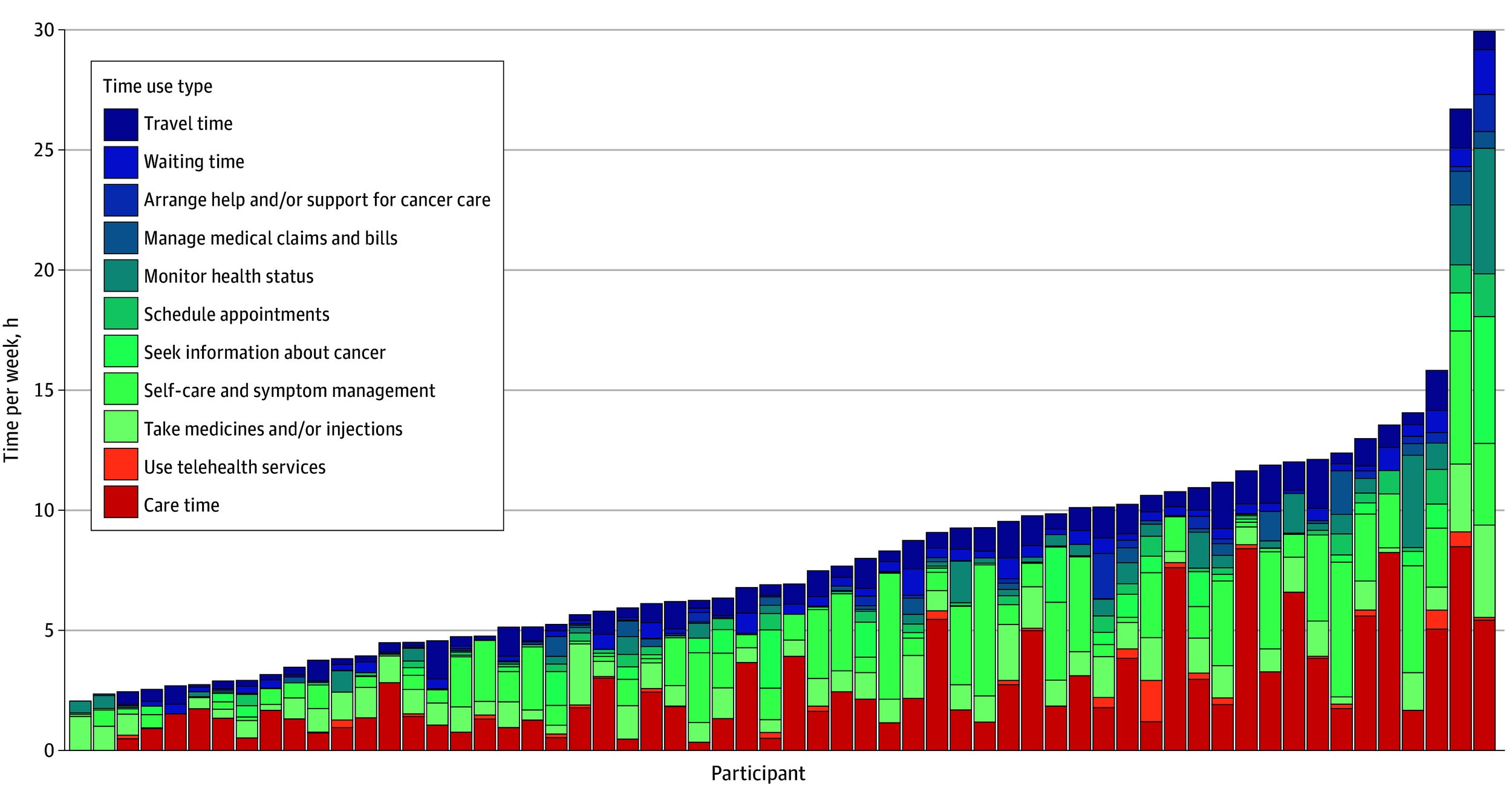
Figure. Weekly Total Time Spent on Each Health Care, Travel Waiting, and Home Cancer-Related Task by Participant.
Each column represents an individual participant. Care time included all time spent out of home at a medical facility and labeled as cancer care; travel and waiting time were associated with these cancer care visits. All other types (taking medications or injections, self care and symptom management, scheduling appointments, monitoring health status, managing medical claims and bills, and arranging help or support for cancer care) were reported in the end-of-day survey as occurring outside of a health care facility.
-
[00:00:39] Victoria: Hi friends, I'm Victoria Goldberg. We're excited to introduce a new series of short segments that we are calling should we deal With as our very colorful title implies. These episodes tackle the real challenges we, as people living with metastatic breast cancer have to face on the regular basis and research around everyday living with this disease.
Jill Tirabassi, a member of our podcast team and a sports medicine and preventive medicine boarded physician who is also living with MBC hosts, introduces, and writes these segments. Jill brings her medical expertise and personal experience to explore topics that matter to our community. Let's hear from Jill.
[00:01:32] Jill Tirabassi: Hello, my name is Jill Tirabassi and welcome to our segment called Shit we deal with shorts where we talk about topics that unfortunately we have to deal with because we are now living with metastatic breast cancer.
I will dive into research, literature, whatever else is out there to try to find some answers and quantify what the data shows about what we're dealing with.
[00:02:06] Jill: In today's shit we deal with shorts. We are gonna talk about time burden. I'm pulling this topic from an article entitled "Time Burden in Patients with Metastatic Breast and Ovarian Cancer From Clinic and Home Demands". This is published in JAMA Network Open, online in December of 2025.
I've thought a lot about the time burden of living with advanced cancer.you hear things like, ah, living with cancer is a full-time job. And actually this was an interesting study where we looked to see, what truly is the time burden, for people living with either metastatic breast or ovarian cancer.
So diving into this study, people were recruited from two sites, either through the University of Minnesota or the University of Alabama, and they completed baseline and follow-up surveys as well as used a mobile phone app to track their time use for 28 days. And the app uses both GPS and phone sensor data to figure out location as well as activity type.
And there's more details on that and you can of course look at the study if you wanna know more. But I found it very interesting that they ended up with a total of 60 patients, half of whom had MBC, , and over half were not working at this point.
Most patients also were in treatment for what they called, recurrence or progression in their disease. So were not on their first line therapy.
There's a neat graph that if you wanna look at, you can go to the link and look at the, different time use types or ways that they spend their time related to their cancer diagnosis um, including things like travel time waiting and the oncologist's office time managing medical claims and bills, monitoring their health, scheduling appointments, looking up information about cancer, et cetera.
So let's talk about the results, the fun part, the patients reported on average, four out of home cancer related episodes, like visiting a clinic or a pharmacy over the 28 days. So roughly we can think of that once a week patients had to go out of their home to do something, that involved most frequently clinic visits and laboratory, so getting your labs done.
Almost half of them reported wait times less than 15 minutes, but 14% reported wait times of over 60 minutes. And I can think of that sometimes when I visited my oncologist in the past, right, like super long wait times. You just, you know, you're gonna be there all day. , I actually a couple weeks ago had a wait time of two and a half hours to get my labs.
The order for the labs had expired and then the faxes didn't go through and poof, you know, two and a half hours later it finally happened for me.
And that was, that was a pretty brutal day too. And so I think we all had those experiences. Thankfully it's not most of the time, but it can happen. I love that they calculated the travel time for some of these visits. On average it was about 35 minutes. The range was 20 to 57 minutes.
In terms of where most of them fell. Obviously there's more people with more or less time than that. And so they actually came out with this statement concluding that the time spent waiting and traveling for care often exceeded the amount of time receiving care.
Most days the participants in the study had a home cancer related task to do , 80% of days. And the median they say was about 209 minutes per week doing cancer related tasks at home. So that means taking medications, scheduling medical bills, symptoms, planning related to cancer appointments.
So it's not too surprising that over one third of the participants said that these cancer related tasks, disrupted their daily activity on, , more than half their days.
This study shows that for most of the people in this study the time per week that they spend dealing with their healthcare, travel, home related tasks is not technically a full-time job, right? We're not talking about 35 to 40 hour weeks for most people. There were two people in this study that were above 25 hours per week.
But the majority, were really in the five to 15 per week, and that's not insignificant. Um. How many hours are spending a week related to our cancer related care to keep ourselves alive?
I've been on several lines of treatment now, and I think there were definitely some easier lines when I was on oral medications with minimal side effects that life felt kind of normal, compared to perhaps some of the other treatment lines, um, you know, where it's maybe a day one, day eight, and that's a 21 day cycle with IV infusions and I'm traveling to get to those chemo sessions.
So, yeah, i'm curious, when you reflect on where you are in your journey, does this resonate with you? I'm glad that people are actually documenting and trying to study this so that we can truly understand what it's like to be living with something like metastatic breast or metastatic ovarian cancer in this case.
And hopefully we can figure out ways to alleviate some of these burdens.
[00:07:32] Jill Tirabassi: OUTRO
And so that ends today's segment on shit we deal with shorts.
I'm pretty nerdy, so once again, feel free to send me any ideas or topics that you might have, and I'll try to dig into some literature or research about 'em so that we can reflect on all the things that we're now stuck dealing with. I hope that you're doing well. Take care. Until next time.